Not collecting for the work you do on your patients is the fastest way to diminishing profits, increased overhead, and ultimately – lower take home income for yourself, the owner.
If you’re one of the administrative team members of a dental practice, and if your bonuses are tied to offices collections, then this affects you as well.
With this video my goal is to show why it pays to be persistent on your collections – meaning, why it’s so important to have your in house team collect the money owed to your practice on a consistent basis.
Collecting what you produce in your practice is the #1 way to make sure you’re getting paid for work you do on patients.
And, If you’re not collecting what you’re producing, you’re working for free.
Instead of outsourcing to a collection agency and have them take 50% of the money owed, it was worth having my in office team go after the patient balances.
I want to tell you about two separate incidents / scenarios of my real patients to make my point of why you shouldn’t rush to send your patients over to a collection agency right away.
By being persistent with your collections, you’ll add to your bottom line without incurring additional costs.
Stick around until the end because I don’t just talk about the problems we ran into with the two scenarios – I’m also going to share what changes we made to make sure the ball isn’t dropped and these things don’t happen again.
For maintaining cash flow in your dental practice, you probably do most of the following to stay on top of collections:
- Collect patient copays at the time you start the work on patients
- Split patient payments for multi-visit procedures (crowns, bridge) into two visits for patient convenience
- Verify insurance benefits and have them correctly entered and attached to patient’s chart
- Offer patient financing for their convenience
- Ensure your claims have correct procedures attached and provide all supporting documentation necessary for processing of the claim….
- You’ve allowed “extra” flexibility in payments for certain established patients who have been with your practice for a long time and spent a good amount of money
- and so on..
But even after doing all the right things, you still end up having patient balances.
These balances may be from the insurances paying less than what you expect, patient not wanting to pay their balance until both primary and secondary insurance has paid, or maybe your front desk collected less than what they should’ve ..
Or, worst, your team just forgot to collect.
Yes, it does happen.
So for the first patient – she has two insurances.
Before starting her work, we had preauthorized all the work by both of her insurances as she requested.
We send the PreAuths to the primary, and then once we got that back we sent those to the secondary.
Once we have in our hand preauthorizations from both plans stating there will be benefits towards her crowns, we moved forward.

So, by adding up whatever the primary insurance is going to pay and whatever the secondary insurance is going to pay – as long as it equals allowable fee for that procedure – we are good to go.
For this patient, we collected nothing from the patient except for $100 because we knew payments from both plans would cover everything.
As we were progressing in her treatment plan, getting paid from the primary and then sending it to the secondary – we did get paid as we had estimated.
Except for the fact that she ended up needing a root canal that was not in the initial treatment plan.
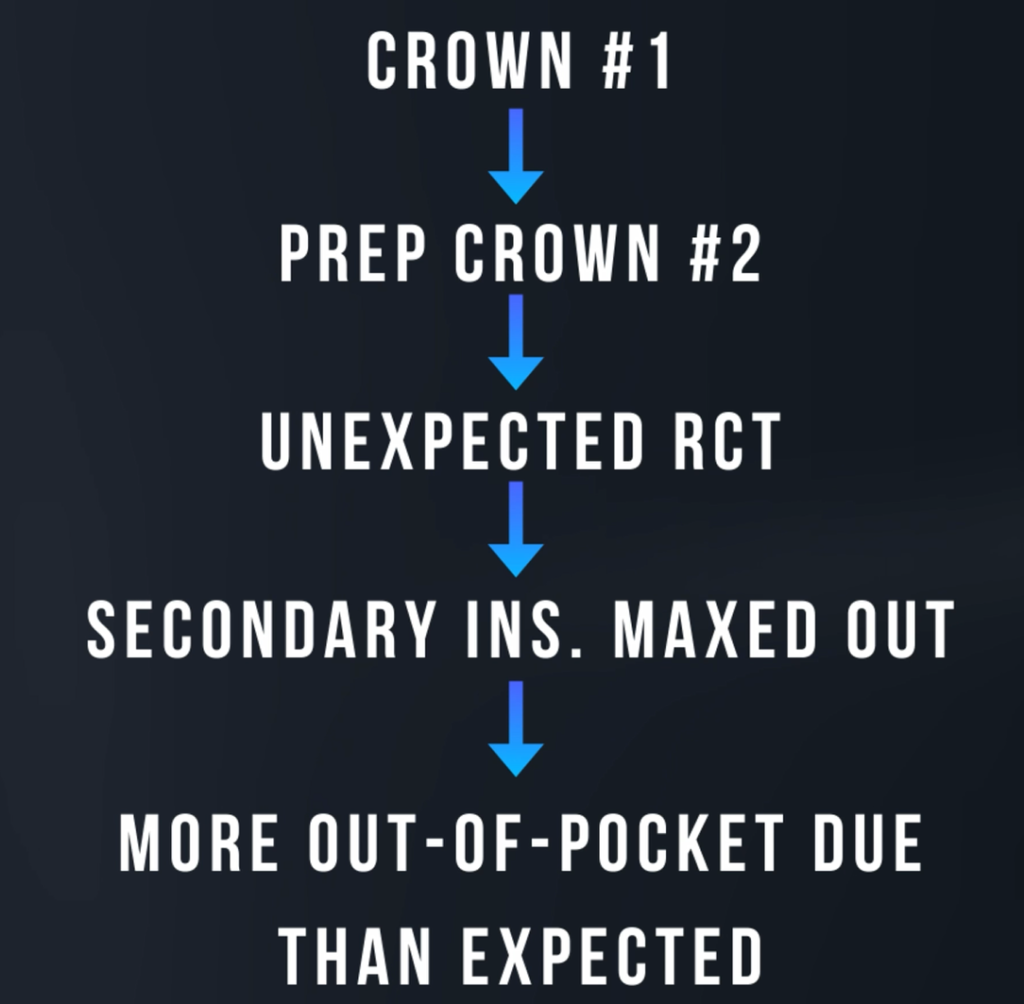
She was informed right away that once she saw the endodontist and prior to starting her last crown, she would be maxed out and she would end up having an out of pocket.
She understood and just wanted the claims filed with both plans first.
As I always discuss, we always stay consistent with our policies to collect at time of service if patient was going to have any out-of-pocket.
However in this case, since she needed the root canal after I had already temporized the tooth and she fractured the tooth and needed a root canal – we decided to wait for the insurance to tell us that she’s maxed out and not collect the $394.50 she was going to owe.
So now all work is done, we’ve received the final EOB from the secondary telling us that she’s maxed out, which leaves her account with a balance.
This is also about one and a half month after work was completed.
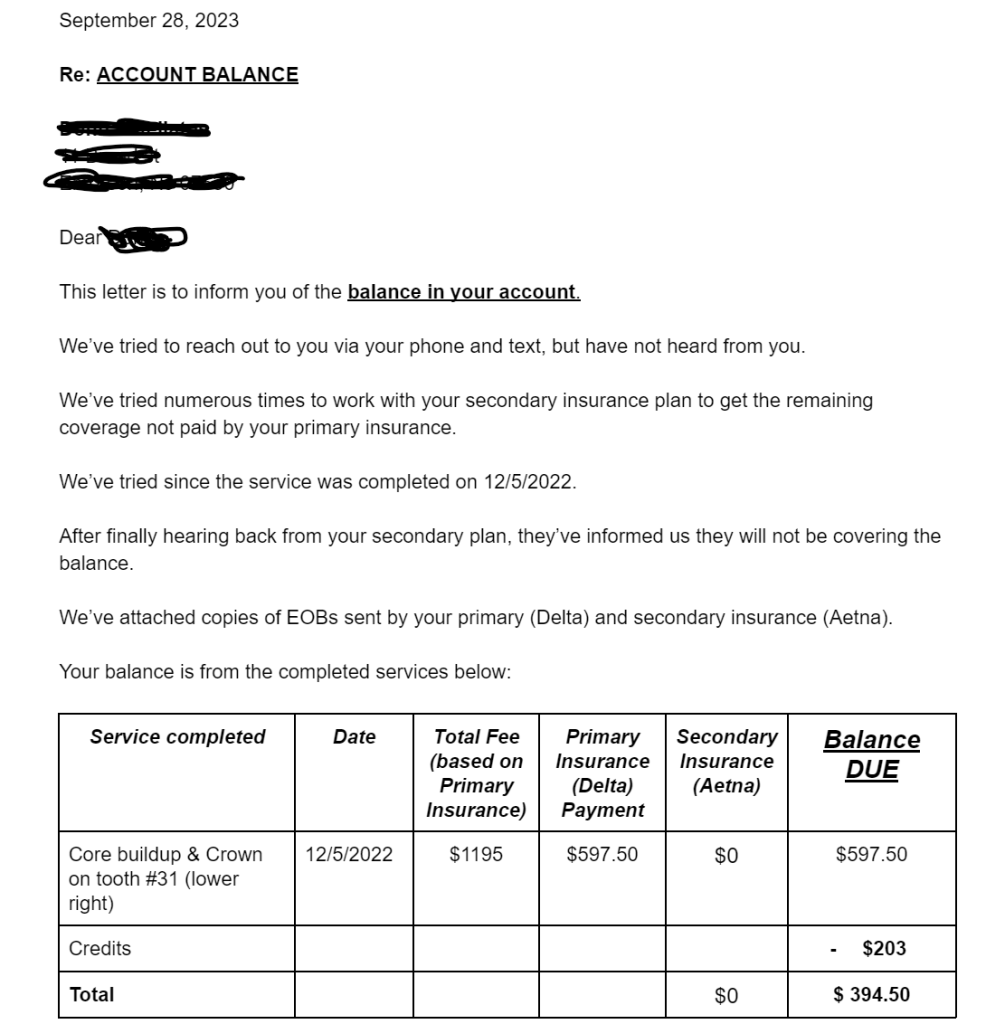
Here’s the template letter that we typically use – we modified it for this case and printed up copies of both primary and secondary EOBs with balance.
Copy of the letter

Primary EOB
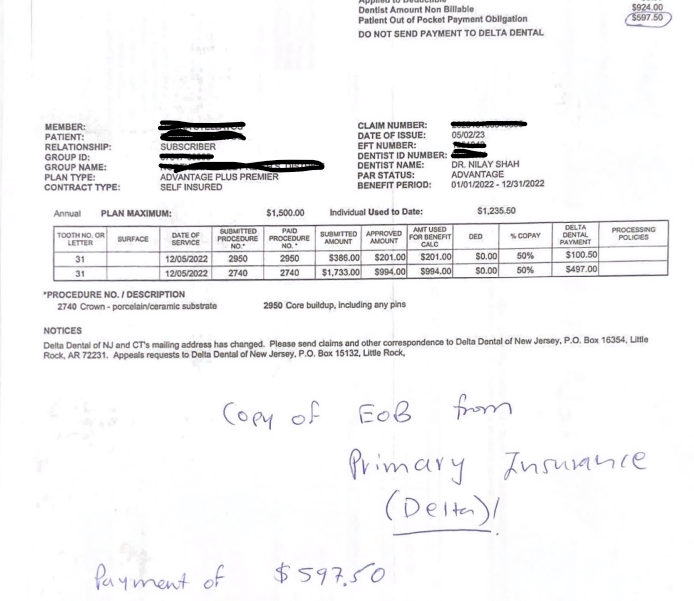
Secondary EOB
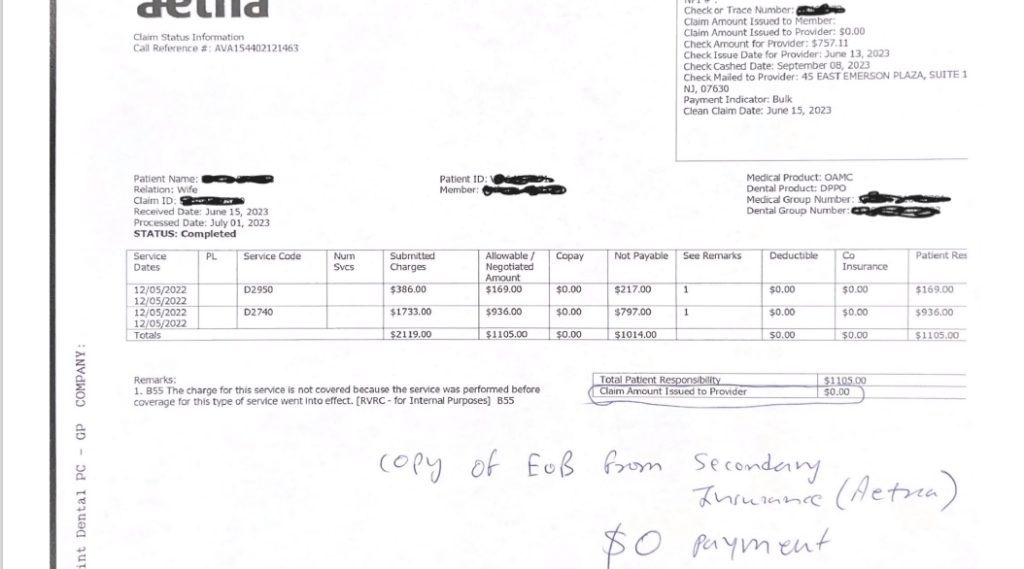

We sent this out in the mail. We left a voicemail for her on the phone letting her know of this.
We don’t hear from her at all.
We sent another statement out the second time about two weeks later.
Then, she did call one day and spoke with my treatment coordinator letting her know she plans on making payments, but didn’t want to make payment at that point on the phone.
Then we don’t hear from her again.
We sent another statement again two weeks later with a “account past due” sticker.
We then called a few days later, and she actually picked up and made a partial payment of $180 over the phone and said she’ll make the rest in some time.
Between quick texts, phone attempts, sending physical statements – on 2/23/2024 she made her final payment bringing her account balance to 0!
Because of the consistent collection efforts, and without sending over to a collection agency, we were able to collect the full money owed to us over time.
You’re probably thinking who has the time to do all that for the whole year – well, actually it wasn’t a ton of work.
The work involved was creating the initial letter and the copy of the EOBs.
But we had a system in place to track when our next attempt to follow-up with her would be – whether it’s through a quick phone call, a text, or mailing a statement.
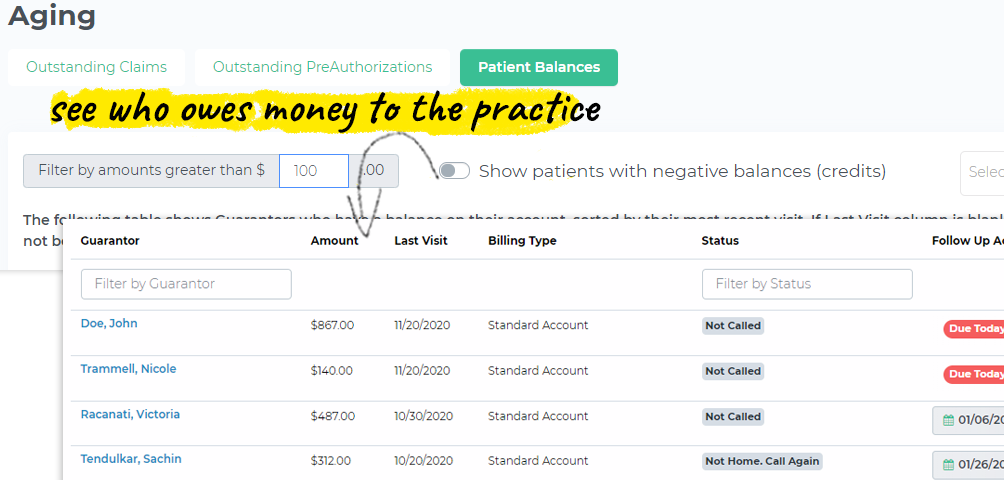
This way, we didn’t have to pull the report of money owed to us again from Open Dental.
It’s right in front of my team member for her to make the next attempt.
The time it takes to actually make the attempt:
- A quick phone call (voicemail because she never picked up) – between dialing and leaving a voicemail – maybe 2 minutes.
- For text – since it’s templated already – less than 30 seconds.
- Mailing a statement: print the letter again with today’s date, put a sticker on it for ATTENTION, fold and stamp the envelope – less than 5 minutes
It was part of the daily routine with the rest of the other tasks that needed to be done – but more importantly, we were consistently in touch.
Let’s talk about another scenario.
Since last year, we’ve had some patients with balances on accounts due to lost checks.
Three of the lost checks were from United Health Care.
When we called to find out whether or not they were cashed – the insurance rep told us they were already cashed.
But, how can that be because they haven’t been entered into Open Dental, and the claim still says pending?
United Health care sent us the image of the cashed check, and I called up the bank whose name was on the back of the check which deposited the check.
I immediately spoke to the manager and they let us know that someone did deposit it.
But they did not want to give us any additional information on whose account it was the checks were deposited into.
When we have physical checks, it has our office stamp in the back.
These checks did not have our stamp, so i know we didn’t deposit it.
The manager said this was a mistake on their part from one of their employees where no one can just deposit the check when it’s made out to our practice.
I called United Health care immediately and they told us we’d have to sign some paperwork etc.
After spending the time to get the documents notarized and sending all the paperwork in, we called three weeks later to find out they have no record on file of them receiving any documents from us.
We again follow up two weeks later, and spoke to a supervisor and they escalated our inquiry to “another higher up”, and they told us they’ll look into it.
There was a follow-up call made every two weeks after that to check the status of these checks, and the only thing we got was “our request is in “processing status”.
At least this was better than hearing that they haven’t received any paperwork from us.
Three full months later, all three checks that we “lost” come in the mail were reprocessed by United Health care and they issued us new checks, which brought the account balance of these specific patients to 0.
Again, this is something that if we didn’t have a system to track which claims were pending and when the follow-up call needed to be made along with the notes of what happened with each follow-up –
There’s NO way my front desk would remember to go back and keep trying to get back the money that’s owed to us – not with all the million things they already feel overwhelmed by at the front.
Lessons Learned
We learned from these mishaps, and decided to make correct changes.
After having gone through the situation of the dual insurances, and looking back on the amount of work we put in, we decided that moving forward, anyone with two insurances, we collect out-of-pocket pretending secondary insurance doesn’t exist.
Once the primary insurance pays and EOBs are sent to the secondary from our office – anything the secondary insurance pays is a complete credit to the patient.
This accomplishes the following:
- We get paid on time.
- We’re still providing an additional service for the patient by filing all paperwork with their secondary plan.
- We reduce work on our end because now we don’t have to track what’s remaining on the secondary insurance in case they’re maxed out from changes in the treatment plan.
If a patient refuses and wants to wait to pay for anything until both plans pay, we just don’t move forward and they can go somewhere else.
I’ve never tried it this way, but that’s how we’re moving forward.
If patients don’t move forward with work because of this, it’s totally fine. I’d rather not deal with chasing for money later.
Implementation
But how do we actually implement this?
Since I’ve started my practice, dealing with two insurances hasn’t really been an issue at all until recently.
Since we’re making this change, how do we implement this within our practice management system – specifically Open Dental?
This requires an extra effort.
If you attach both insurances to a patient’s chart – Open Dental will automatically calculate no patient out-of-pocket since both plans are attached.
In order to ignore the secondary plan, and have Open Dental calculate copays correctly, drop the secondary plan temporarily on the day patient comes in, so your front desk knows what to collect for the work being done that day.
However, the problem with this method is that you cannot drop a plan if a pending claim is still attached to a patients chart, which maybe the case because you’re generating claims for the secondary insurance for the work that’s being completed.
So the way around this problem is this:

Keep only the primary plan attached to a patient’s chart.
Do all work needed to complete the treatment plan.
Send claim only for primary and don’t attach the secondary plan.
This way you’ll be able to see what to charge the patient for their copay assuming only the primary plan.
Once all the work is done and primary claims have been paid – you can go back and attach the secondary plan and generate claims for the dates the patient came in.
Because you already collected patient copays at the time of service – anything that’s paid by the secondary insurance from this point on, would be a credit back to the patient.
Since the recording of this video, we’ve already done this with few patients and have had no resistance or problems from patients wanting to move forward with treatment.
They’re simply happy that we’ll be filing all the paperwork for them with their secondary after everything’s done to get them some money back.
Regarding the second scenario with the lost checks, we decided that we want to move away completely from receiving paper checks from all plans,
So since then, we have now completely switched over to EFT – which are payments directly into bank from the insurance companies.
But, this has added an extra step in our process of entering checks into our practice management system.
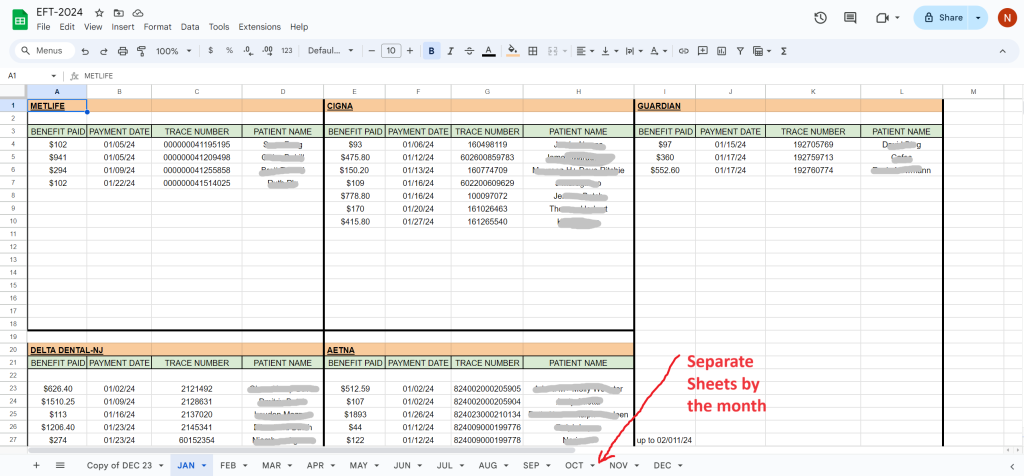
We now have an excel sheet to track all claims that are entered via eft from the insurance portal.
The excel sheet just tracks by the month when payments are made, by which insurance companies, the payment amount, trace number of the payment, and the patient.
This is then reconciled with the actual payments that ends up in the bank for checks and balances.
Alright, moving on.
Don’t delay Collections
An important factor in trying to collect on owed balances is the amount of time that has passed since the patient has had a balance on their account.
When we talk about accounts receivables, the “industry standard” is to look at 30-60-90.
It’s simply referring to account balances that are more than 30 days old, more than 60 days old and more than 90 days old.
Keeping an eye on AR should be part of your daily / weekly and monthly routines for your front desk team.
If you’re doing it consistently, majority of the times your balances shouldn’t go past the 30 days.
But in reality, some do go over 30 days into range of 30-60 days.
But older the account balances, harder it is to collect!
But it doesn’t mean you shouldn’t go after it.
For the two scenarios I discussed earlier, those balances were way past the 120 days, but we were still able to collect in full without handing over to a collection agency.
Older balances are harder to collect because
- It’s out of the patient’s mind, so they’re not getting back to you right away.
- Your team is doing more work by following up with them, phone calls, sending statements, etc.
- In some cases, if the time lapse is too long, the chance of you collecting anything from the accounts drops significantly.
So, it’s always better to reach out to patients right away as soon as the balance is there on their account and keep following up until it’s paid in full.
Don’t send to collection agency so fast:
We could’ve sent these patients over to a collection agency.
But we didn’t.
Once the patient is sent to collections, you chance of actually collecting that money drops to something like 10%.
And the collection agency can take up to 50% of what they actually collect.
By having a system to help you track your collection efforts and know when it’s time to follow-up again – you’re increasing the chance of actually reaching the patient.
Majority of the time, the actual work is TRACKING everything –
- What was sent,
- What was said,
- When the phone call happened,
- When the letter was sent,
- When’s the next time to reach out, etc.
When your team is busy doing gazillion things like answering patient phone calls, checking patients in and out, scheduling appointments – all of this is time consuming.
How do you possibly have your team member reach out to the claim they called three weeks ago about a lost check?
And that’s just one. What about the 10 other pending claims from two months ago that need follow-ups because some of them didn’t receive the documentation they need to process the claims.
How do you note all that down so someone actually remembers to do it and actually forward it to someone, for instance, if you need a narrative for a claim, or maybe the claim got denied and you may want to speak with the consulting doctor to appeal, etc.
Unless you have a way to get your team to see pending money on a consistent basis – the important work is just not going to get done.
And then you wonder why your collection doesn’t meet the production and WHY your take home isn’t what you expect when you’re busy producing
That’s it for today guys. I hope this was helpful.
Take your collections seriously, implement a system that is easy for your team to follow so they can do it consistently.
By adding friction to the process, you’ll make it difficult for your team and they’re less likely to keep up with AR balances.